Finding a suspicious spot on your skin can be scary, but the timing of your discovery changes everything. For those who catch Melanoma is a malignant tumor originating from melanocytes, the pigment-producing cells in the skin early, the 5-year survival rate is over 99%. However, if it's not found until it spreads, that number drops to around 32.1%. This massive gap is why the shift toward AI-powered screening and advanced immunotherapy isn't just a trend-it's a literal lifesaver.
How Early Detection is Changing
For decades, we relied on the "ABCDE" rule and a doctor's eye. While that still matters, the tools are getting much sharper. We're moving away from simple visual checks toward technology that can "see" what a human eye misses. Current standards usually start with a visual inspection, followed by dermoscopy, which uses a handheld magnifier to look deeper into the skin's layers.
But the real game-changer is the arrival of Artificial Intelligence (AI). Researchers at Northeastern University developed the SegFusion framework, which uses a two-step process: first, it isolates the lesion, then it classifies it. This system has hit 99% accuracy in certain tests. Why does this matter? Because it helps doctors avoid the common problem of "dataset bias," where AI struggles with different skin tones or lighting. By isolating the spot first, the AI can focus on the actual cellular patterns rather than the background skin.
Then there are the non-invasive gadgets. The DermaSensor, cleared by the FDA in early 2024, uses Elastic Scattering Spectroscopy. Instead of just taking a photo, it shoots near-infrared light into the skin to see how it scatters. If the light bounces back in a certain way, it suggests cancer. It's designed for primary care doctors who aren't skin specialists, giving them a high-tech "second opinion" during a routine checkup.
| Method | Sensitivity (Catch Rate) | Specificity (Accuracy of "Negative") | Best For... |
|---|---|---|---|
| Visual Inspection (GP) | 60-70% | 65-75% | Initial triage |
| DermaSensor (ESS) | 85-95% | 26-40% | Primary care screening |
| AI (SegFusion/DenseNet) | 95%+ | 87%+ | Specialist confirmation |
The Future of Screening: Wearables and Full-Body Scans
Imagine a world where you don't have to wait for a yearly appointment to check your back. Wake Forest University is working on a wearable patch that measures bioimpedance. Basically, it checks the electrical properties of your skin. Cancerous tissue conducts electricity differently than healthy skin. While it's still in early testing with small groups, the goal is a battery-free device that can alert you to changes in a mole in real-time.
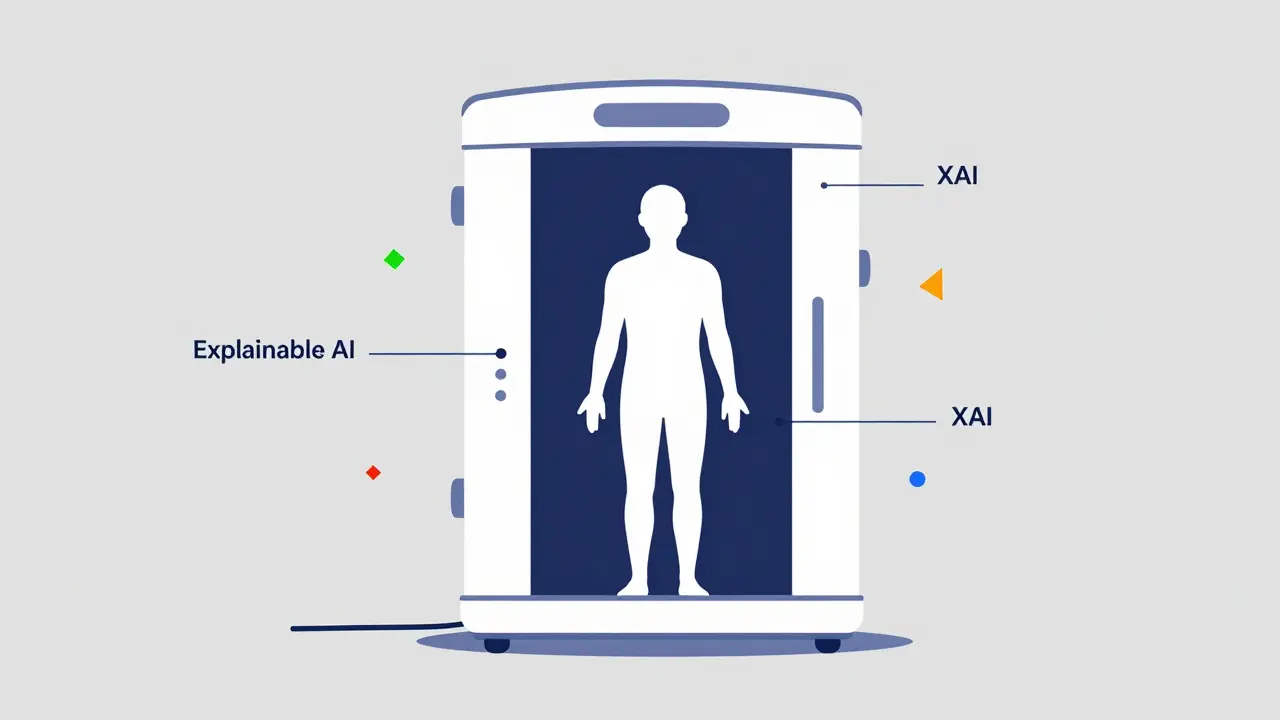
For those who want a comprehensive look, the iToBoS project in Europe has created a full-body scanner. It can map your entire skin surface in about six minutes. It uses Explainable AI (XAI), which means it doesn't just say "this is cancer"-it shows the doctor the specific reasons why it flagged a spot. This transparency helps dermatologists trust the machine and reduces the chance of missing a small, hidden lesion on the scalp or between toes.
Modern Immunotherapy: Teaching the Body to Fight
Once melanoma is detected, especially if it has reached a metastatic stage, the focus shifts from surgery to Immunotherapy. Unlike chemotherapy, which attacks all fast-growing cells, immunotherapy tells your own immune system to stop ignoring the cancer.
The big breakthrough happened with drugs that target the PD-1 and CTLA-4 pathways. Think of these as "brakes" on your immune system. Cancer cells often flip these brakes "on" so your T-cells don't attack them. Drugs like Ipilimumab and newer PD-1 blockers flip those brakes "off," allowing your immune system to recognize and destroy the tumor.
We are now entering the era of personalized cell therapy. The SUPRAME Phase 3 trial is currently testing IMA203 PRAME cell therapy. This isn't a one-size-fits-all drug; it's designed for patients with a specific genetic marker (HLA-A*02:01). In early phases, this approach showed a 56% complete objective response rate, which is a massive win for patients with unresectable tumors.

The Trade-off: Overdiagnosis and Anxiety
It's not all good news. With these hyper-sensitive AI tools, we face a new problem: overdiagnosis. When a tool like the DermaSensor has a specificity of only 26-40%, it means it flags a lot of benign moles as potentially dangerous. This leads to more biopsies. While a biopsy is a simple procedure, doing it unnecessarily causes stress and physical scarring.
There's also the issue of the "digital divide" in medicine. Many current AI models were trained on datasets that don't include enough diverse skin tones. Some studies show these systems can perform 12-15% worse on darker skin. Until the data becomes as diverse as the people using the tools, we have to be careful not to rely solely on the algorithm.
Practical Steps for Your Next Checkup
If you're heading to a dermatologist, don't just let them glance at you. Be proactive about the tools they use. Ask if they utilize AI-assisted imaging or dermoscopy for high-risk areas. If you have a family history of skin cancer, ask about full-body mapping, which creates a baseline of your moles so the doctor can see exactly which ones change over time.
Keep an eye on your own skin using the "Ugly Duckling" sign. While the ABCDEs are great, the Ugly Duckling method is often more intuitive: look for the one spot that looks and feels completely different from all the other moles on your body. If one spot doesn't "fit in," that's the one that needs a professional look.
How often should I get screened for melanoma?
For most people, a yearly professional skin check is a good baseline. However, if you have a fair complexion, a history of severe sunburns, or a family history of melanoma, your doctor might recommend checks every 3 to 6 months. Those with immunosuppressed systems should be screened even more frequently.
Is immunotherapy better than chemotherapy for melanoma?
In many cases, yes. Immunotherapy targets the immune system's ability to fight cancer and often has a more durable response. While chemotherapy kills cells indiscriminately, immunotherapy (like PD-1 and CTLA-4 inhibitors) helps the body maintain a long-term defense. However, it can cause unique side effects called immune-related adverse events, where the immune system attacks healthy organs.
Can AI actually replace a dermatologist?
Not yet. Current AI tools are designed as "decision support systems." They are excellent at flagging suspicious areas and reducing human error, but they lack the clinical judgment to consider a patient's full medical history and the tactile feel of a lesion. The best results come from a "human-in-the-loop" approach where AI finds the spot and the doctor confirms the diagnosis.
What should I do if I find a new mole?
Don't panic, but don't ignore it. Note when you first saw it and take a clear photo with a ruler next to it to track size. Look for changes in color, irregular borders, or any itching or bleeding. Schedule a dermatology appointment and specifically mention that you've found a "new or changing lesion" to get a priority slot.
Are there any at-home AI apps for skin cancer?
There are several, but use them with extreme caution. Most consumer apps aren't FDA-cleared for diagnosis and can give a false sense of security. They are okay for tracking changes via photos, but they should never replace a professional biopsy or clinical exam by a board-certified dermatologist.

Written by Felix Greendale
View all posts by: Felix Greendale